Last updated: April 13, 2026
Quick Summary: Most morning constipation routines focus on what you eat or drink. This one starts with your nervous system — because without first shifting your body from “fight-or-flight” into “rest-and-digest,” nothing you take will work reliably. This sequence activates your vagus nerve, primes your gut motility reflex, and creates the neurological conditions your colon needs to move. The steps matter more than the clock — adapt the timing to your body, but keep the sequence. Consistently done, it retrains your gut-brain axis over 4–8 weeks.
You wake up. Before you’ve even gotten out of bed, you’re already bracing.
Will today be a good day or a bad day?
That question — that anticipatory anxiety about your morning bathroom routine — is not just a thought. It is a physiological event. The moment you begin dreading your gut, your brain activates a low-level stress response. Cortisol rises. Your vagus nerve quiets. Your colon, which needs a clear “safe to move” signal from your nervous system to initiate its natural contractions, receives silence instead.
And then you wonder why the magnesium isn’t working today.
I spent 15 years starting my mornings this way. What finally changed things wasn’t a new supplement. It was changing what I did first — and understanding why the sequence mattered more than the schedule.
Why Your Morning Is the Most Important Window for IBS-C
What is the morning gut-brain window? The 30–60 minutes after waking is the most important period for gut motility in people with IBS-C. Two natural mechanisms are strongest at this time: the gastrocolic reflex (triggered by eating or drinking, which sends a movement signal to the colon) and the migrating motor complex (the gut’s natural housekeeping wave). If your nervous system is in a stress state when you wake, both reflexes are suppressed before your day has even started.
Your body runs on circadian rhythms — biological clocks that govern when different systems are most active. For your gut, the morning is peak motility time. Cortisol naturally rises after waking (this is called the cortisol awakening response), and in a regulated nervous system, this morning cortisol spike actually supports gut motility by stimulating the gastrocolic reflex.
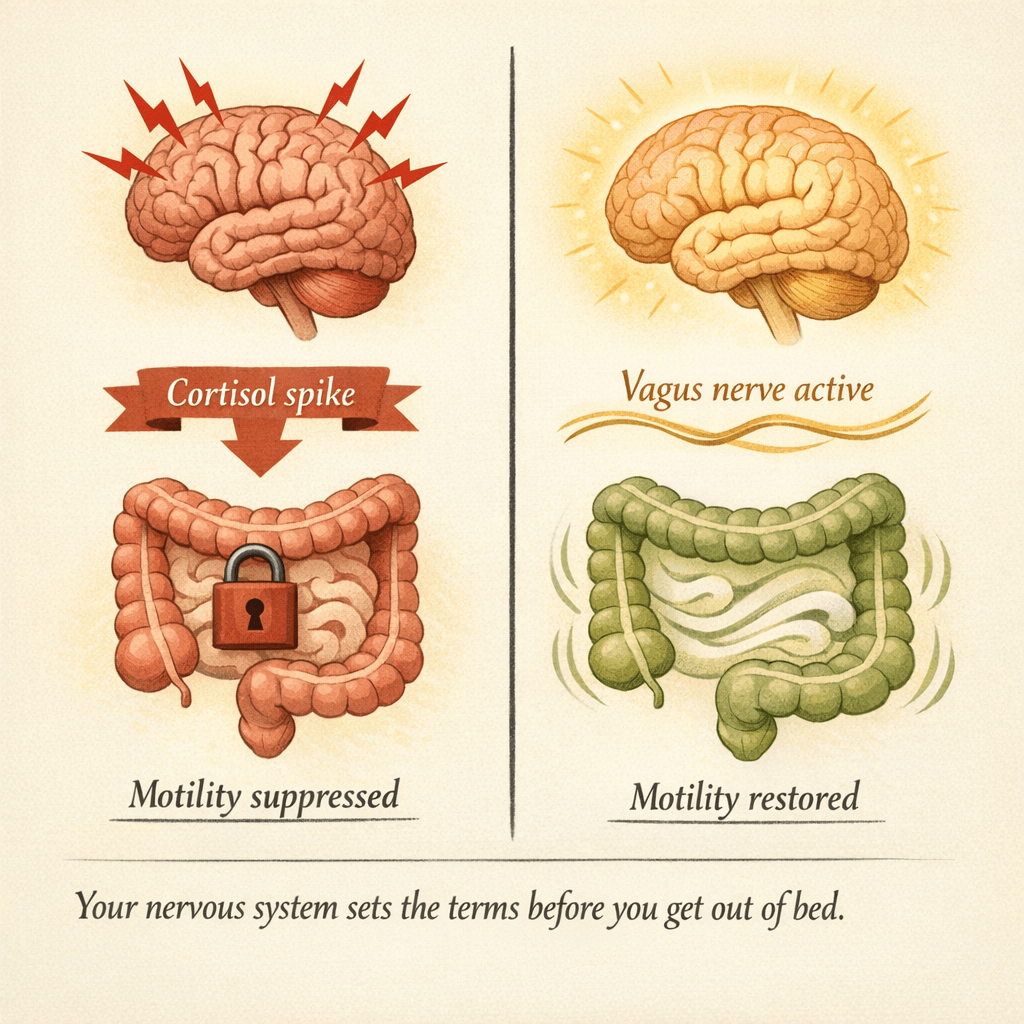
But here is the problem for chronic constipation sufferers: if your baseline cortisol is already elevated from chronic stress, this morning spike tips you over into sympathetic dominance — the “fight-or-flight” state — instead of activating digestion. The signal gets crossed. Your colon reads “danger” instead of “move.”
This is why so many women with IBS-C notice that their gut works better on holidays or weekends — and worse on Monday mornings. It is not random. It is your nervous system setting the terms.
The key insight: You cannot supplement your way out of a nervous system in fight-or-flight mode. The morning routine below doesn’t add more supplements. It changes the neurological state your supplements enter.
The Morning Routine: A Sequence, Not a Schedule
This routine has four steps. The sequence matters — each step creates the physiological conditions for the next one to work. The timing is flexible. You don’t need a stopwatch. What you need is to do them in the right order, every morning.
My own morning looks like this: I take a few slow breaths before reaching for my phone, then make coffee and eat some fruit, and somewhere around 15 minutes later my body signals it’s ready. The routine doesn’t have to be formal or rigid — it needs to be consistent.
Step 1: Before Your Phone — Set Your Nervous System
Before you sit up, before you check messages, before you assess how your stomach feels: take one slow breath.
Inhale through your nose for 4 counts. Exhale through your mouth for 6 counts.
Do this just three times, lying in bed.
Why this matters: The moment you pick up your phone, your brain begins processing social information, notifications, and the day’s demands — all of which can trigger a low-level stress response within seconds. That response elevates cortisol and activates your sympathetic nervous system before you have even stood up. Three slow exhale-extended breaths before anything else sends the first “safety” signal of the day to your vagus nerve, creating a parasympathetic window to build on.
My personal tip: I keep my phone on the other side of the room specifically for this reason. Even if you don’t do that, the few slow breaths before reaching for it make a genuine difference to how your morning unfolds.
Step 2: The Vagus Nerve Activation
Once you’re sitting or standing, spend a few minutes on deliberate slow breathing. You don’t need to time it precisely — a few cycles done with intention is enough.
The technique: Inhale through your nose → hold briefly → exhale slowly through your mouth, making the exhale longer than the inhale. The 4-7-8 pattern (inhale 4, hold 7, exhale 8) works well, but the key principle is simply: exhale longer than you inhale. Repeat 4–6 times, or for however long feels natural.
Why this works: The extended exhale is the active mechanism. Exhalation activates the parasympathetic nervous system via the vagal brake — a neural mechanism that slows heart rate and signals safety to the brainstem. A 2022 systematic review in Neuroscience & Biobehavioral Reviews (Laborde et al.) confirmed that voluntary slow breathing with extended exhalation measurably increases vagally-mediated heart rate variability — the most reliable marker of vagal tone — both during practice and after. A 2021 study in Scientific Reports (Magnon et al.) found that just 5 minutes of this type of breathing significantly increases parasympathetic activity and reduces perceived anxiety.
Higher vagal tone means your vagus nerve is more active. An active vagus nerve sends the “rest-and-digest” signal your colon needs to initiate its motility reflex.
You can do this while making your coffee, sitting at your kitchen table, or standing by a window. It does not require a meditation cushion or silence. The goal is not perfection — it is parasympathetic activation.
My personal tip: On mornings when I feel particularly anxious, I hum on the exhale instead of breathing out silently. The vocal cord vibration directly stimulates the vagus nerve branches in the throat, and I find it creates an even faster shift in how my body feels. Try it — it sounds strange but it works.
Step 3: The Gut Trigger — Warm Drink and Light Food
This is where your morning coffee, tea, or warm water comes in — and where a light breakfast fits naturally into the sequence.
Have your warm drink. Eat something light if that’s your pattern — fruit, a small bowl of oats, whatever your body is used to. Take your morning supplement here if you use one: magnesium citrate or a tablespoon of olive oil or MCT oil works best taken alongside or just after something warm.
Why this works: Warm liquid entering the stomach and food stretching the stomach wall trigger the gastrocolic reflex — a neurological response where the stomach signals the colon to initiate a peristaltic wave. According to StatPearls (NIH), the gastrocolic reflex is most active in the morning and immediately after meals, making this the physiologically optimal window to reinforce the motility habit. Coffee in particular is a well-documented gastrocolic reflex trigger — both caffeinated and decaffeinated versions stimulate gastrin release, which enhances the reflex.
Crucially, your supplement now enters a gut that is in a parasympathetic state — primed and receptive — rather than a gut in stress-driven shutdown. The breathing you did in Step 2 is what makes this step more effective.
My personal tip: I add a small pinch of sea salt and a squeeze of lemon to my warm water on days when I skip coffee. The electrolytes support the electrical signaling in the colon walls, and the slight acidity of lemon mildly stimulates digestive secretion. But honestly — if coffee works for you, coffee is perfect.
Step 4: The Bathroom Appointment
Within 20–30 minutes of eating or drinking, go to the bathroom. Not because you feel an urgent urge — but because you have a standing appointment with your gut.
Sit with a footstool under your feet so your knees are raised above your hips. This straightens the anorectal angle by relaxing the puborectalis muscle — the muscle that, in a standard seated position, creates a kink in the rectum that makes elimination harder. The squatting position removes that kink mechanically.
Once seated: breathe. Do not strain. Do not check your phone. Give your body whatever time it needs — some mornings that’s 5 minutes, some mornings it’s 10. Some mornings nothing happens, and that is completely fine.
Why this works: Your defecation reflex is a neurological habit, not just a physical event. Like all habits, it strengthens through consistent repetition at the same time and under the same conditions. Neurologically, this is called a conditioned reflex — your enteric nervous system learns to expect a bowel movement when a specific set of cues is presented consistently. Research on circadian gut function confirms that colonic motility is significantly higher in the post-breakfast window, making this the physiologically optimal time to reinforce the habit.
The footstool matters. Studies using defecography show that a squatting position reduces the time needed for complete evacuation and reduces the straining force required. For IBS-C sufferers with pelvic floor tension — a common co-occurrence with anxiety — this mechanical advantage is significant.
My personal tip: Some mornings nothing happens. I kept a simple tick chart for my first month: one tick per morning I showed up at the bathroom, regardless of outcome. That unbroken streak was more motivating than any single successful bowel movement. You are building a neurological rhythm over weeks, not performing a task each morning.
The Sequence at a Glance
| Step | What You Do | What It Does |
|---|---|---|
| First | 3 slow breaths before your phone | Sets parasympathetic baseline before cortisol spike |
| Second | Slow breathing with extended exhale × 4–6 cycles | Activates vagus nerve, raises HRV, switches to rest-and-digest |
| Third | Warm drink + light food + morning supplement | Triggers gastrocolic reflex; supplement enters a primed gut |
| Fourth — within 20–30 min of eating | Bathroom appointment with footstool | Reinforces conditioned defecation reflex via consistent timing |
Why Consistency Matters More Than Any Single Morning
The most common mistake with this routine is treating it like a rescue tool — something to use on bad days. That is not how nervous system retraining works.
Your vagal tone — the baseline strength of your vagus nerve signaling — is built through repeated, daily practice. Think of it like a muscle. One good session doesn’t build strength. Thirty consistent sessions do. The same principle applies to your gut-brain axis.
Here is what to expect as you build the habit:
Week 1–2: The routine feels unfamiliar. Some mornings will show no gut response. This is normal — your nervous system needs repetition before it changes its baseline. Focus on showing up, not on results.
Week 3–4: You begin to notice pattern shifts. Some mornings feel easier. The breathing starts to feel less effortful. Your gut may begin to respond more consistently to the food and supplement trigger.
Week 5–8: The conditioned reflex begins to establish. Your body starts to anticipate the bathroom appointment. Anxiety around the morning routine begins to soften because you are building a track record of predictability — and predictability is safety to your nervous system.
Week 9–12: New baseline established. The routine becomes automatic. Emergency episodes become less frequent. The nervous system has learned a new pattern.

Frequently Asked Questions
How long does it take for a morning routine to help IBS-C?
Most people notice the first pattern shifts within 2–3 weeks of consistent daily practice — not dramatic relief, but a reduction in morning anxiety and occasional easier eliminations. Meaningful, reliable improvement in gut motility typically develops over 4–8 weeks. Full nervous system retraining — where the conditioned morning reflex becomes automatic and emergencies become rare — takes 8–12 weeks. The timeline depends on how long the nervous system dysregulation has been present and how consistently the routine is practiced.
Does the order of the steps matter?
The sequence matters more than the exact timing. The core principle is simple: nervous system first, gut trigger second, bathroom third. Breathing before your drink or breakfast primes your gut to respond. Eating or drinking something warm then naturally triggers the gastrocolic reflex — which is why many people find that coffee or a light breakfast does the same job as warm water in this routine.
In practice, there is real flexibility in how you layer the steps. My own morning looks like this: a few slow breaths, then coffee and some fruit (with either one spoon of MCT oil or Olive oil), and around 15 minutes later my body signals it’s ready. The breathing doesn’t need to be a formal seated practice — it can happen alongside your morning drink.
What matters most is consistency in the overall pattern: calm nervous system → food or drink trigger → bathroom at roughly the same time each morning. Don’t let the structure of this routine become another source of morning anxiety. Adapt it to what feels natural for your body while keeping the core sequence intact.
What if I have no urge at all in the morning — should I still sit?
Yes — and this is exactly the point. The bathroom appointment works precisely because you are not waiting for an urge. You are creating the neurological conditions for an urge to develop over time. In IBS-C, the defecation reflex is often suppressed or desensitized. Waiting for a natural urge before attempting a bowel movement can mean waiting indefinitely, which reinforces the suppressed reflex. Showing up consistently — even without urgency — is the training that gradually restores the conditioned reflex. Do not strain. Simply sit, breathe, and allow.
Can I do this routine if I take prescription medications?
The breathing practice and bathroom timing are safe for everyone and do not interact with medications. For the supplement component — magnesium citrate or oils — consult your doctor if you are on prescription medications. Magnesium can affect the absorption timing of some drugs, particularly thyroid medications and certain antibiotics. This routine is for educational purposes and is not medical advice.
Your Next Steps
If you are starting this routine today, here is where to go next on NeuroSpirit:
→ Understand why your supplements stop working: Why Constipation Remedies Stop Working (And My 3-Step Rotation Protocol to Fix It)
→ The science behind the vagus nerve and your gut: The Vagus Nerve Blockade: Why Chronic Stress Literally Stops Your Digestion
→ For emergency days: Emergency Constipation Relief: A 3-Step Science-Backed Plan
The free 7-Day Vagus-Vital Starter Guide walks you through the nervous system foundation step by step — so you can stop the guesswork and start building a gut-brain rhythm that actually holds.
👉 Enter your email below to get instant free access.
Sources
- Johns Hopkins Medicine — The Brain-Gut Connection
- Polyvagal Institute — Polyvagal Theory: Stephen Porges
- Scientific Reports — Benefits from One Session of Deep and Slow Breathing on Vagal Tone and Anxiety (Magnon et al., 2021)
- Neuroscience & Biobehavioral Reviews — Effects of Voluntary Slow Breathing on HRV: A Systematic Review and Meta-Analysis (Laborde et al., 2022)
- NIH StatPearls — Physiology: Gastrocolic Reflex
- NIH Office of Dietary Supplements — Magnesium: Health Professional Fact Sheet
- American Journal of Physiology — Squatting Position and Defecation Studies
About the Author
Ting is a gut-brain health writer and the founder of NeuroSpirit, a resource for people navigating the intersection of the nervous system and digestive health. She has managed IBS-C herself for over 15 years, which drives her commitment to translating clinical research on the gut-brain axis into practical, experience-tested strategies. Her writing bridges the gap between gastroenterology, nervous system regulation, and daily life for people who have been told their constipation is “just stress.”
Disclaimer: This post shares insights from my 15-year journey with IBS-C and is for educational purposes only. It is not medical advice. Please consult your doctor before making any changes to your diet, supplements, or health routine.


Leave a comment