Last updated: April 13, 2026
Quick Summary: You can’t tell which came first — the anxiety or the constipation. That’s because neither came first. They are locked in a bidirectional biological loop, each one feeding the other through the gut-brain axis. This post explains exactly how that loop forms, why standard advice fails to break it, and the nervous-system-first protocol that interrupts it at the root.
You notice it every time. Your anxiety spikes — and within hours, your gut locks up. Or you’ve been constipated for days — and the discomfort starts feeding your anxiety. You can’t tell anymore which came first.
This is not a coincidence. It is not weakness. It is not something you are imagining.
It is the constipation-anxiety loop — a real, documented biological cycle where gut dysfunction and nervous system dysregulation reinforce each other through the gut-brain axis. Understanding how it works is the first step to breaking free from it.
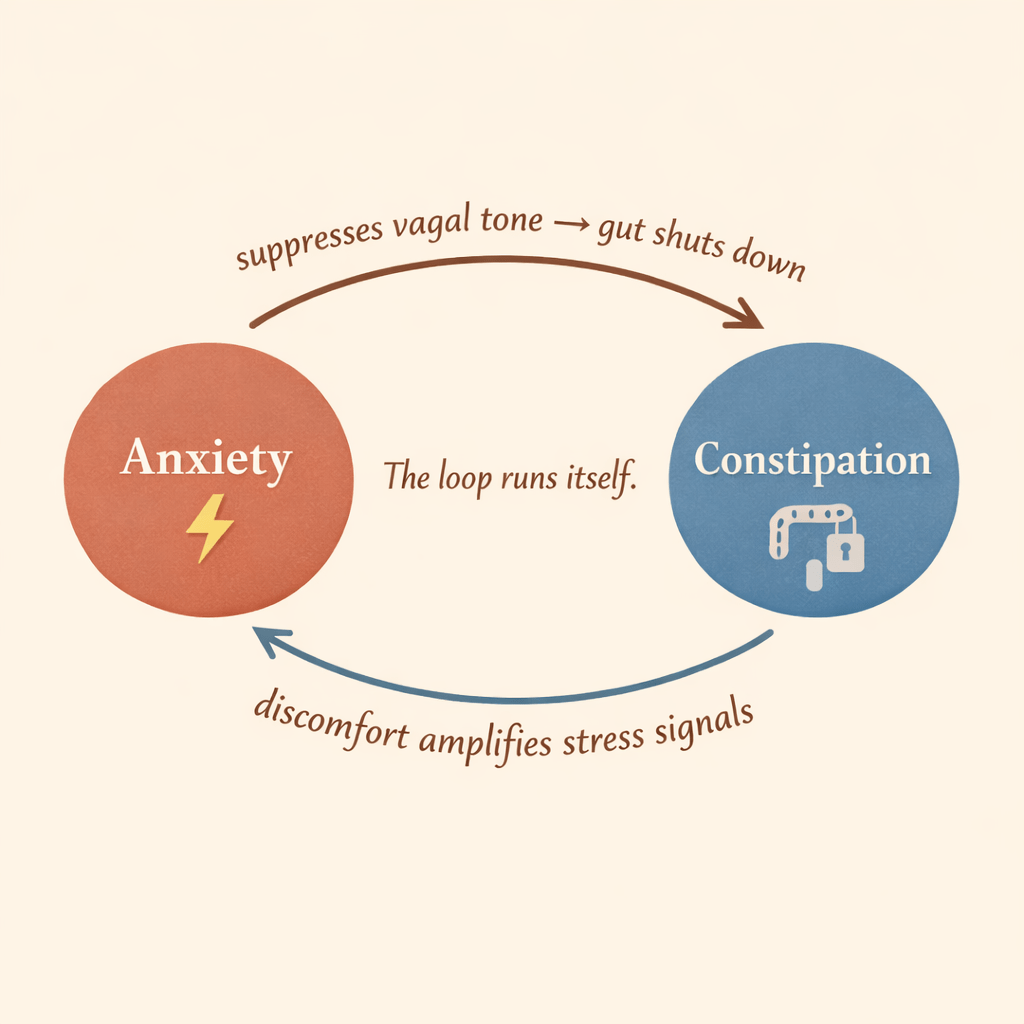
What is the constipation-anxiety loop? The constipation-anxiety loop is a bidirectional cycle in which anxiety activates the sympathetic nervous system, suppressing gut motility and causing constipation, while constipation itself generates physical discomfort and worry that further elevates anxiety. The two conditions reinforce each other through the vagus nerve and the gut-brain axis, making it difficult to resolve either one without addressing both simultaneously.
Why Standard Advice Keeps Failing
Most constipation advice targets one end of this loop — usually the gut. Drink more water. Eat more fiber. Take a laxative. These approaches can provide temporary relief, but they don’t interrupt the loop because they ignore the nervous system that is running it.
Most anxiety advice has the same problem in reverse — it targets the mind without addressing the gut signals that are amplifying the stress response.
Breaking the loop requires working both ends of the axis at the same time. That is exactly what this protocol does.
How the Loop Forms: The Science
1. The Vagus Nerve Goes Quiet
Your vagus nerve is the primary communication highway between your brain and your colon. When it is active — when your parasympathetic nervous system is in charge — it sends a continuous “safe to digest” signal that keeps gut motility running smoothly.
Chronic stress suppresses this signal. Elevated cortisol dampens vagal tone, slowing the migrating motor complex (the gut’s natural housekeeping wave) and reducing colon motility. The result is constipation — not from a structural problem, but from a nervous system that has decided digestion is not a priority right now.
Research published in PLOS ONE confirmed that IBS patients show a measurable uncoupling between vagal tone (measured by heart rate variability) and cortisol levels compared to healthy controls — meaning the normal regulatory relationship between the parasympathetic nervous system and the stress response is disrupted in people with IBS (Pellissier et al., 2014).
2. The Bacterial Balance Shifts
A slow-moving gut creates conditions where bacteria can overgrow and produce inflammatory metabolites. These metabolites can travel through the gut lining and affect mood, cognition, and anxiety levels — completing a feedback loop that started in the nervous system and now runs through the microbiome as well.
3. Serotonin Signaling Gets Disrupted
Approximately 95% of the serotonin in the body resides in the gut Badgut, where it plays a critical role in regulating motility and gut-brain signaling. People with IBS-C who experience constipation often have lower levels of serotonin, and the muscles in their rectums are less reactive to serotonin — making them more likely to have hard or lumpy stools. Healthline
This matters for anxiety because serotonin is also a key mood-regulating neurotransmitter. When gut serotonin signaling is disrupted by constipation and inflammation, the downstream effects reach the brain — amplifying the anxiety that started the loop in the first place.
4. The Anticipatory Anxiety Layer
Once you have experienced a bad constipation day, your brain begins to anticipate the next one. This anticipatory anxiety — dreading your morning routine before it begins — activates a low-level sympathetic stress response that suppresses vagal tone before you have even gotten out of bed. The loop now runs before anything has physically happened. This is one of the most important and underappreciated mechanisms in IBS-C.
The loop in plain terms: Anxiety suppresses vagal tone → gut motility slows → constipation develops → discomfort and worry amplify anxiety → vagal tone drops further → constipation worsens. No supplement interrupts this from the outside. The interruption has to come from inside the nervous system.
The 4-Step Protocol to Break the Loop
Healing requires working both ends of the axis: calming the nervous system to help the gut, and supporting the gut to calm the nervous system. Here is how to do both simultaneously.
Step 1: Activate Your Vagus Nerve — Send Safety Signals First
Before anything else in your morning, signal safety to your nervous system. This is the step most people skip — and it is the most important one.
Diaphragmatic breathing with extended exhale: Inhale slowly through your nose, then exhale through your mouth for longer than you inhaled. Even 3–5 slow cycles before reaching for your phone or assessing your gut begins to raise vagal tone and lower the cortisol response.
The physiological sigh: Inhale fully, take one more small sip of air on top, then exhale completely and slowly. This double-inhale technique rapidly deflates the air sacs in the lungs and has been shown to produce a fast reduction in physiological stress arousal. Use it during moments of acute anxiety — it works within seconds.
Humming: The vagus nerve passes through the vocal cords. Humming on the exhale creates vibrations that directly stimulate vagal branches in the throat. You can do this while making coffee or standing in the shower.
None of these require dedicated meditation time. They work alongside your normal morning activities.
Step 2: Nourish With Foundational Support
Once your nervous system is primed, your supplements enter a gut that is physiologically ready to respond. Timing and sequence matter here — nervous system first, then support.
Magnesium Citrate (200–400mg) — morning, on rotation: Works osmotically, drawing water into the colon to soften stool and stimulate movement. Rotate with olive oil or MCT oil rather than taking daily — this prevents receptor adaptation. See the full Rotation Protocol for the exact schedule.
High-quality olive oil or MCT oil (1 tablespoon) — on rotation days: Triggers the gastrocolic reflex via fat-stimulated bile release — a completely different mechanism from magnesium, which is why rotating between them keeps both pathways responsive.
Omega-3s (EPA/DHA): Reduces systemic inflammation that disrupts gut-brain signaling. Multiple studies link omega-3 supplementation to reduced anxiety symptoms, making this the supplement that works on both ends of the loop simultaneously.
Step 3: Support With Smart Fiber
Fiber works — but only when your gut motility is already running. Adding fiber to a stressed, shutdown gut adds bulk without movement, which worsens bloating and discomfort.
Start with soluble fiber only — psyllium husk or ground flaxseed. Soluble fiber forms a gel rather than adding bulk, making it gentler on a gut with impaired motility. Start with a small amount and increase slowly. Introduce fiber after you have been doing the nervous system work for at least 1–2 weeks, not before.
Avoid insoluble fiber (wheat bran, raw vegetables in large quantities) until motility has improved. The engine needs to run before you add cargo.
Step 4: Build the Mind-Gut Rhythm
Consistency is what retrains a conditioned reflex. The loop was built through repeated associations (stress → gut shutdown). Breaking it requires building a new association (calm → gut moves) through equally repeated practice.
Eat in a calm state. Eating while stressed activates the sympathetic nervous system, which suppresses the gastrocolic reflex — the very reflex you need to initiate a bowel movement. Even 3 slow breaths before a meal changes the neurological state your digestive system enters.
Establish consistent meal and bathroom timing. Your enteric nervous system learns from repetition. Eating at roughly the same times each day and sitting on the toilet at the same time each morning — even without urgency — gradually builds a conditioned defecation reflex. For the full morning sequence, see The Morning Routine That Retrains Your Gut-Brain Axis.
Move gently every day. A 20–30 minute walk stimulates the vagus nerve through rhythmic movement, improves colonic motility directly, and reduces anxiety. It is the single lifestyle intervention that works on all three drivers of the loop simultaneously.

What to Expect as You Break the Loop
The loop was not built in a day. Breaking it takes consistent repetition over weeks, not dramatic effort on any single day.
Week 1–2: The nervous system begins to receive new signals. Some mornings will feel easier. The anxiety around the morning routine may begin to soften slightly. Supplements may feel more effective.
Week 3–4: A pattern starts to emerge. Good days begin to outnumber bad ones. The breathing practice feels less effortful and more automatic.
Week 5–8: The conditioned reflex strengthens. Emergency episodes become less frequent. The anticipatory anxiety — the morning dread — begins to diminish because you are building a track record of predictability.
Week 9–12: New baseline established. The loop has been interrupted. This does not mean every morning will be perfect — it means the crisis pattern is no longer the default.
Frequently Asked Questions
Can anxiety actually cause constipation, or does constipation cause anxiety?
Both — simultaneously. This is what makes the loop so hard to break with single-direction treatments. Anxiety activates the hypothalamic-pituitary-adrenal (HPA) axis, elevating cortisol and suppressing vagal tone, which directly slows gut motility. The resulting constipation and bloating then generate their own anxiety — particularly anticipatory anxiety about the next morning. Neither condition is the root cause. The loop itself is the problem, which is why both ends must be addressed at the same time.
Why doesn’t fiber help my constipation if I also have anxiety?
Because fiber requires active motility to move through the colon. When your nervous system is in chronic fight-or-flight mode, the migrating motor complex — the wave that propels fiber through your gut — is suppressed. Adding more bulk to a system without adequate movement creates more bloating and discomfort without improving transit. Nervous system regulation must come first. Fiber becomes much more effective once vagal tone is restored and motility has improved.
How long does it take to break the constipation-anxiety loop?
Most people notice the first meaningful shifts within 2–4 weeks of consistent nervous system work — reduced morning anxiety, more reliable bowel rhythm, supplements feeling more effective. Full cycle-breaking, where emergency episodes become rare and the morning dread has lifted, typically takes 8–12 weeks. The timeline reflects how long the nervous system needs to unlearn a deeply practiced pattern of alarm and build a new pattern of safety.
Is this approach safe to use alongside medication for anxiety or IBS?
The nervous system practices — breathing, consistent routine, gentle movement — are safe alongside all medications and have no interactions. For supplements, check with your doctor if you are on prescription medications, as magnesium can affect absorption timing of certain drugs. This post is for educational purposes and is not medical advice.
Your Next Steps
→ Start with the morning sequence: The Morning Routine That Retrains Your Gut-Brain Axis
→ Understand the vagus nerve: The Vagus Nerve Blockade: Why Chronic Stress Literally Stops Your Digestion
→ Stop supplement adaptation: Why Constipation Remedies Stop Working (And My 3-Step Rotation Protocol)
The free 7-Day Vagus-Vital Starter Guide walks you through the nervous system foundation step by step — so you can stop the guesswork and start building a gut-brain rhythm that actually holds.
👉 Enter your email below to get instant free-guide access:
Sources
- PLOS ONE — Vagal Tone, Cortisol and IBS: Relationship Between Vagal Tone, Cortisol, TNF-Alpha, Epinephrine and Negative Affects (Pellissier et al., 2014)
- Bad Gut / Dr. Michael Gershon — IBS and Serotonin: 95% of Serotonin in the Gut
- Healthline / PubMed — How Serotonin in the Brain Affects Your Bowels
- PMC — Role of Serotonin in the Pathophysiology of IBS
- Johns Hopkins Medicine — The Brain-Gut Connection
- Polyvagal Institute — Polyvagal Theory: Stephen Porges
- NIH StatPearls — Physiology: Gastrocolic Reflex
About the Author
Ting is a gut-brain health writer and the founder of NeuroSpirit, a resource for people navigating the intersection of the nervous system and digestive health. She has managed IBS-C herself for over 15 years, which drives her commitment to translating clinical research on the gut-brain axis into practical, experience-tested strategies. Her writing bridges the gap between gastroenterology, nervous system regulation, and daily life for people who have been told their constipation is “just stress.”
Disclaimer: This post shares insights from my 15-year journey with IBS-C and is for educational purposes only. It is not medical advice. Please consult your doctor before making any changes to your diet, supplements, or health routine.

Leave a reply to Magnesium for IBS-C: Citrate vs. Glycinate (How It Affects Constipation, Anxiety & Sleep) – Finding the Science in SpiriT Cancel reply