Last updated: April 6, 2026
Quick Answer: Chronic stress suppresses vagus nerve activity through sustained cortisol elevation, which directly shuts down gut motility — causing constipation that doesn’t respond to fiber, water, or diet changes. The vagus nerve is the primary parasympathetic pathway between your brain and colon. When it’s blocked by stress, your gut stops receiving the “safe to digest” signal entirely. Restoring vagal tone through breathwork, humming, and nervous system regulation is the first step — before any supplement will work reliably.
What is the vagus nerve blockade? The vagus nerve blockade is the suppression of vagus nerve activity caused by chronic stress and elevated cortisol. Because the vagus nerve is the body’s primary “rest-and-digest” pathway — running from the brainstem to the colon — its suppression directly halts gut motility, peristalsis, and digestive secretion. In people with IBS-C, this creates constipation that is neurological in origin, not dietary.
Have you ever wondered, “Why am I always constipated, even when I’m eating enough fiber, drinking plenty of water, and doing everything ‘right’?”
You’re not alone. Millions struggle with chronic constipation that defies simple dietary fixes. The missing piece isn’t in your kitchen—it’s in your nervous system.
If you’re someone who feels constantly wound up, anxious, or “on alert,” and your gut feels just as stuck as your thoughts, this is for you. Today, we’re diving deep into the biological link between a stressed brain and a frozen gut: the vagus nerve blockade.
The Desperate Loop: Anxiety, Stress, and a Gut That Won’t Move
First, let’s name the frustrating reality many face:
- You’ve tried the prunes, the extra salads, the gallon water bottles.
- You feel bloated, sluggish, and mentally foggy.
- The harder you try to “fix” your gut, the more anxious you get about it.
- You feel stress in your shoulders, your jaw, and… your silent, unmoving colon.
This isn’t a failure of willpower. It’s a failure of signaling. Your brain and gut are having a communication breakdown, and the main cable connecting them – the vagus nerve – is on mute.
Your Nervous System’s Two Modes: The Real Cause of “Frozen Gut”
To understand the fix, you need to understand the two primary states your nervous system cycles between:
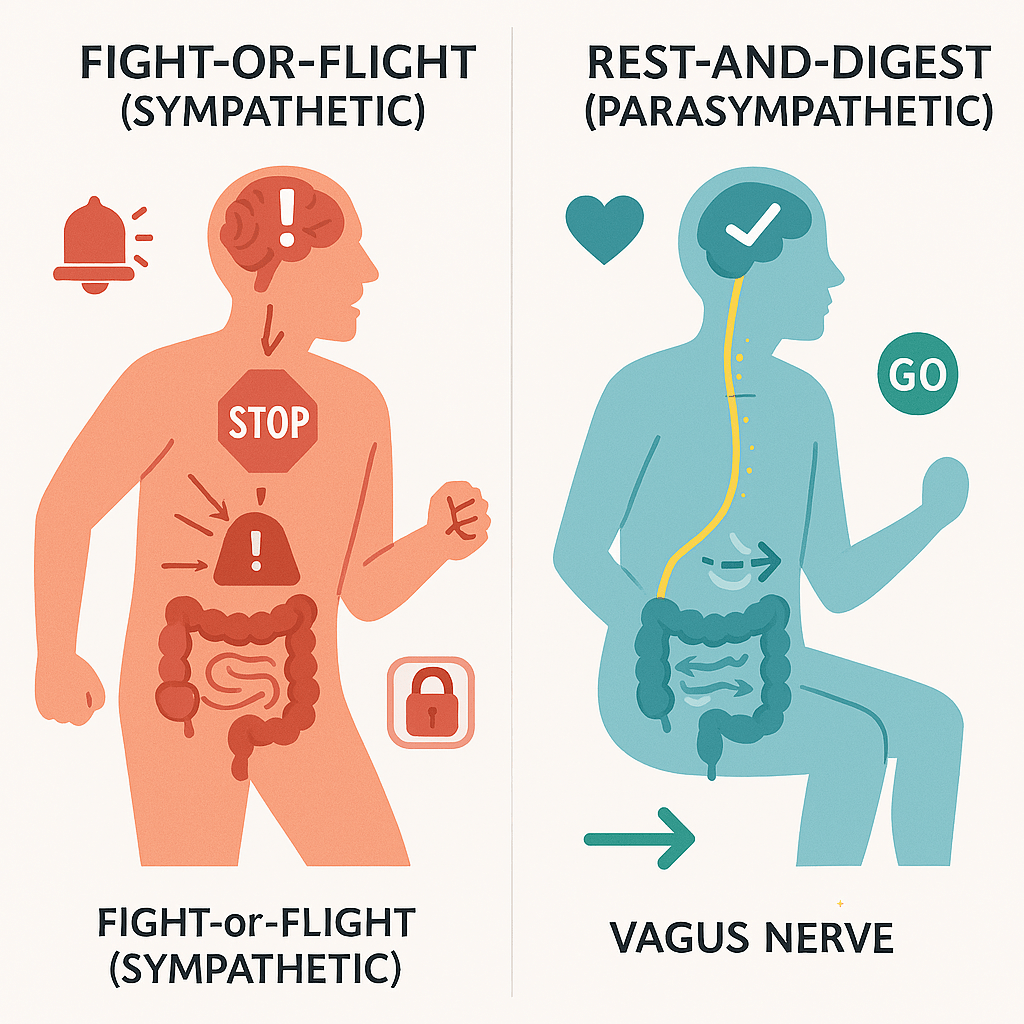
1. Fight-or-Flight (Sympathetic State):
This is your body’s emergency broadcast system. When your brain perceives stress, whether it’s a looming deadline, financial worry, or even chronic anxiety about your health – it flips this switch. Resources are diverted away from “non-essential” maintenance tasks. Your heart rate increases, muscles tense, and yes, digestion completely shuts down. Research from Harvard Medical School confirms that the enteric nervous system — the gut’s own neural network — contains over 500 million neurons and is directly regulated by the autonomic nervous system. Under sympathetic activation, colonic motility can decrease by up to 40% within minutes of a perceived stressor. Why? Your body thinks it’s running from a tiger. It doesn’t have time to process lunch.
2. Rest-and-Digest (Parasympathetic State):
This is the state of calm, repair, and, crucially, digestion. When you’re safe and relaxed, your body turns its energy toward long-term projects: healing, immune function, and moving food through your gut. The master conductor of this “Rest-and-Digest” orchestra is the vagus nerve.
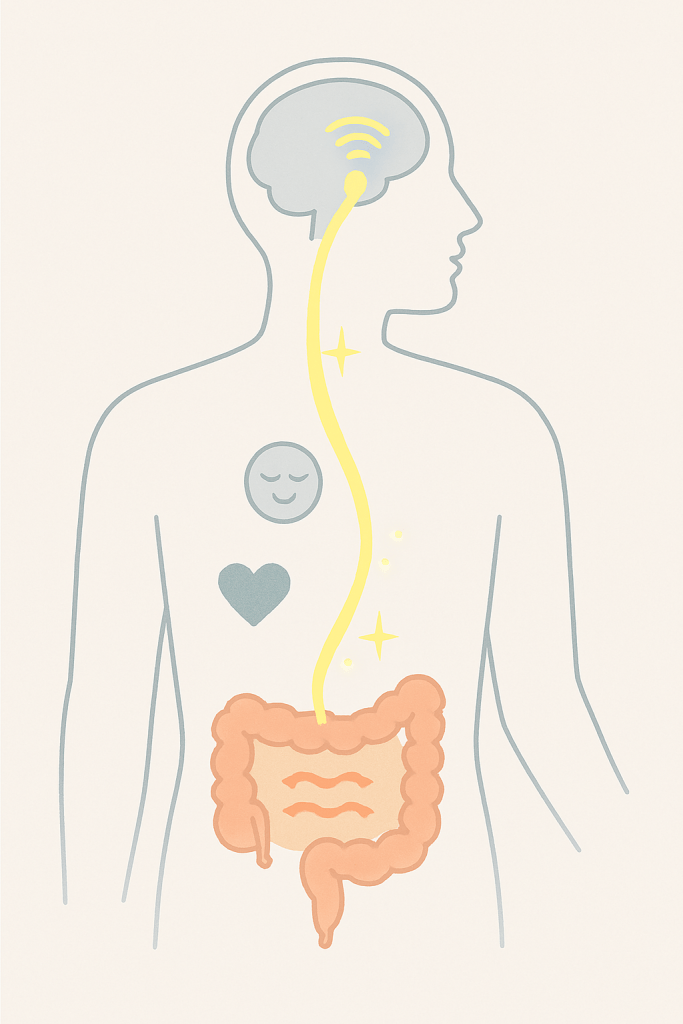
The Vagus Nerve: Your Gut-Brain Superhighway (Now Under Construction)
The vagus nerve is the longest cranial nerve in your body. It’s a two-way communication superhighway running from your brainstem to your colon, touching your heart, lungs, and every major digestive organ.
Its job in digestion is simple but vital: to send the “all clear” signal.
When the vagus nerve is toned and active, it’s like a gentle, constant massage for your digestive tract, stimulating muscle contractions (peristalsis) that move waste along. It tells your stomach to release acid and your intestines to process nutrients.
But here’s the blockade: Chronic stress and anxiety suppress vagus nerve activity. A 2020 study published in Frontiers in Psychiatry found that individuals with chronic anxiety disorders showed significantly lower heart rate variability (HRV) — the gold standard measurement of vagal tone — compared to healthy controls. Low HRV is directly correlated with slower colonic transit time in IBS-C patients. It’s like your brain is putting a “DO NOT DISTURB” sign on the door to your gut. No signal goes down. Without that vagal tone, your intestinal muscles get weak and uncoordinated. The result? Sludge-like movement, bloating, and constipation that feels impossible to resolve with food alone.
Why This Feels So Hopeless
This explains why the standard advice often fails:
- More Fiber? If your gut is paralyzed, adding more bulk can just create a bigger traffic jam.
- More Water? Without muscular movement to push things along, water gets absorbed earlier in the tract.
- More Stress: The desperation from not finding a fix adds more anxiety, further suppressing your vagus nerve, tightening the loop.
You’re not broken. You’re stuck in a biological state that prioritizes survival over elimination.
Does this sound like your story?
Everything failed. Then I stopped treating my gut.
I put together a free 7-day guide that walks through exactly what finally worked for me after 15 years of IBS-C — a nervous system reset that has nothing to do with fiber, diets, or supplements that stop working.
👉 Enter your email below and I’ll send it straight to you. Free.
The First Step Isn’t a Supplement—It’s a Signal
The goal isn’t to force your gut to move with harsh stimulants. It’s to switch your nervous system out of “fight-or-flight” and into “rest-and-digest.” You need to manually reset the signal.
Simple, science-backed ways to begin stimulating your vagus nerve today:
- Diaphragmatic Breathing: 5 minutes of deep, slow breaths (inhale 4 counts, exhale 6 counts). This directly activates vagal pathways.
- Humming or Singing: The vagus nerve passes through your vocal cords. A clinical study found that regular humming and chanting practices measurably increased HRV in participants over a 4-week period — suggesting consistent vocal vagal stimulation creates cumulative, not just immediate, improvements in parasympathetic tone. Humming creates vibrations that stimulate it.
- Cold Exposure: A splash of cold water on your face or a 30-second cold shower can trigger the “diving reflex,” which boosts vagal tone.
Vagus Nerve Stimulation Methods: Quick Comparison
| 4-7-8 Breathing | Humming / Singing | Cold Exposure | Consistent Morning Routine | |
|---|---|---|---|---|
| How it works | Extended exhale directly activates parasympathetic nervous system via respiratory vagal afferents | Vibration through vocal cords stimulates vagal branches in the throat | Triggers diving reflex — rapid parasympathetic activation via facial nerve and vagus | Trains the gut-brain axis to expect a safe, predictable morning signal |
| Speed of effect | 3–5 minutes | 5–10 minutes | 30–60 seconds | Cumulative over 2–4 weeks |
| Best for | Acute stress before bathroom routine | Daily vagal toning practice | Breaking a freeze/shutdown state | Long-term motility retraining |
| Evidence level | Strong — multiple RCTs on HRV improvement | Moderate — emerging research on vocal vagal stimulation | Moderate — diving reflex well established | Strong — consistent timing shown to improve gastrocolic reflex |
| How to use for IBS-C | 5 minutes every morning before supplements | Hum while making morning tea or coffee | Cold water on face before toilet routine | Same bathroom time daily, post-breakfast |
Frequently Asked Questions
What is the vagus nerve and why does it affect digestion?
The vagus nerve is the longest cranial nerve in the body, running from the brainstem through the neck, chest, and abdomen to the colon. It is the primary pathway of the parasympathetic nervous system — the “rest-and-digest” state. In digestion, the vagus nerve sends the signal that triggers peristalsis (the muscle contractions that move stool), stimulates stomach acid release, and coordinates the gastrocolic reflex after eating. When vagal tone is suppressed by chronic stress, all of these functions slow or stop.
Can stress really cause constipation?
Yes — through a direct physiological mechanism, not just a psychological one. Chronic stress elevates cortisol, which suppresses vagal tone and shifts the autonomic nervous system into sympathetic dominance. In this state, blood flow is diverted away from the digestive tract, colonic motility slows, and the migrating motor complex — the wave-like contraction that clears the colon — is inhibited. Research shows colonic transit time can slow significantly within minutes of sympathetic activation, making stress one of the most measurable drivers of constipation in IBS-C.
How do I know if my constipation is nervous system related?
Key signs that your constipation is nervous-system driven rather than purely dietary: it worsens predictably during stressful periods, it doesn’t improve with fiber or water increases, it comes with bloating that feels like “tension” rather than gas, you have a history of anxiety or chronic stress, and standard laxatives work temporarily but the pattern always returns. If all of these apply, the root cause is likely vagal suppression — not diet, not microbiome, not fiber intake.
How long does it take to improve vagal tone?
Measurable improvements in heart rate variability — the standard marker of vagal tone — have been shown in clinical studies after 4–8 weeks of consistent daily practice (breathwork, humming, or cold exposure). For gut motility specifically, many people notice a shift in bowel consistency and morning rhythm within 2–3 weeks of daily 4-7-8 breathing. Full nervous system retraining for chronic IBS-C typically takes 8–12 weeks of consistent practice.
What’s Next? Introducing the Chemical “Off-Switch”
Learning to manually stimulate your vagus nerve is the foundation. But for many whose systems are deeply locked in stress mode, the body needs a clearer biochemical signal to truly relax and reset.
In our next post, we’ll reveal the #1 mineral that acts as your nervous system’s natural “chill pill.” It’s a critical co-factor for hundreds of enzymatic processes, including those that produce calming neurotransmitters and directly relax the smooth muscle of your intestinal tract. It’s the missing key for turning off the “fight-or-flight” alarm at a cellular level, so your vagus nerve can finally do its job.

Sources
- Harvard Medical School — The Gut-Brain Connection
- Polyvagal Institute — Polyvagal Theory: Stephen Porges
- Frontiers in Psychiatry — Heart Rate Variability and Anxiety Disorders
- Frontiers in Human Neuroscience — Vagal Tone and Gut Motility in IBS
- NIH National Library of Medicine — Autonomic Nervous System and Colonic Motility
- Johns Hopkins Medicine — The Brain-Gut Connection
If nothing has worked — this is why.
“Everything Failed. Then I Stopped Treating My Gut.”
Free 7-day nervous system reset guide for women with chronic constipation whose doctors have run out of answers. The exact approach that broke my 15-year cycle — and the science explaining why it works.
👉 Enter your email for instant free access.
About the Author
Ting is a gut-brain health writer and the founder of NeuroSpirit, a resource for people navigating the intersection of the nervous system and digestive health. She has managed IBS-C herself for over 15 years, which drives her commitment to translating clinical research on the gut-brain axis into practical, experience-tested strategies. Her writing bridges the gap between gastroenterology, nervous system regulation, and daily life for people who have been told their constipation is “just stress.”
Disclaimer: This post shares insights from my 15-year journey with IBS-C and is for educational purposes only. It is not medical advice. Please consult your doctor before making any changes to your diet, supplements, or health routine.

Leave a comment